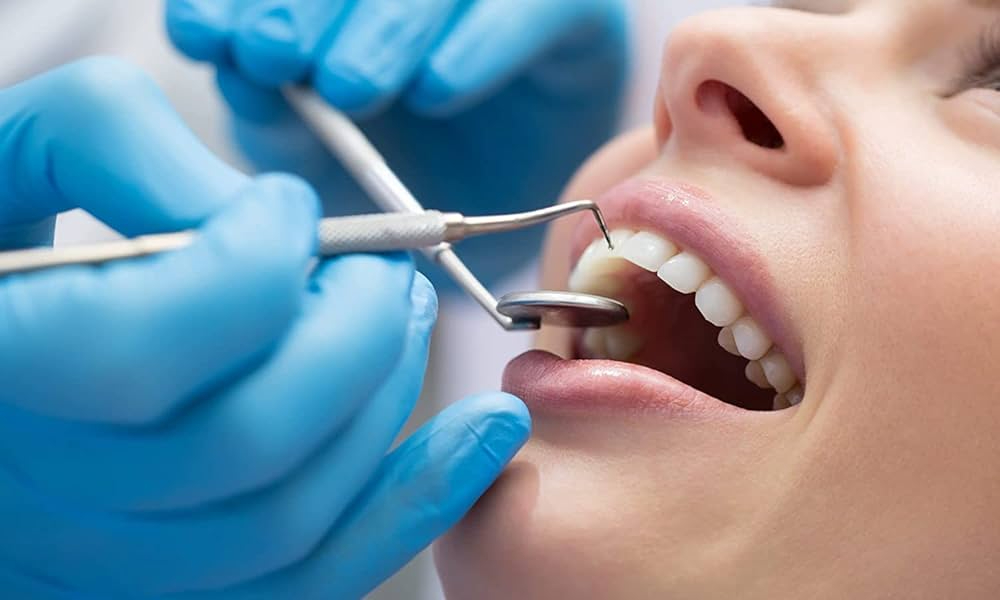
Facing oral maxillofacial surgery can shake your sense of control. You may worry about pain, recovery, or how your face will look. You may feel rushed and unheard. You deserve clear answers before you agree to anything. This blog explains what happens before, during, and after surgery. It shows how your surgeon plans your care, manages pain, and guards your safety. It also walks through common procedures, from wisdom teeth removal to jaw correction. Every step has a purpose. Every step has risks and benefits. You will see what questions to ask and what details matter. You will also learn how to prepare your body and your home, so you heal with fewer surprises. If you get care at firewheel dentistry garland tx or any other clinic, you can use this guide to speak up, stay informed, and protect your health.
What Oral Maxillofacial Surgeons Do
You meet an oral maxillofacial surgeon when a regular dentist cannot safely fix a problem. These surgeons treat your mouth, jaws, and face. They focus on bone, teeth, and soft tissue.
Common reasons you may see one include:
- Impacted or painful wisdom teeth
- Jaw pain or trouble chewing
- Facial injury or broken jaw
- Missing teeth that need implants
- Cysts, growths, or infection in the jaw
Before Surgery: Your Evaluation Visit
The first visit shapes your whole care plan. You should leave that visit with clear next steps.
You can expect three basic parts.
- Medical history review. You share health problems, past surgeries, and all medicines. You include pills, insulin, inhalers, blood thinners, and supplements.
- Exam and imaging. The surgeon looks at your mouth and face. Then you may get X-rays or 3D scans.
- Treatment plan talk. The surgeon explains what needs to happen, how long it will take, and what it will cost.
Bring a written list of:
- Your medicines and doses
- Allergies to drugs or latex
- Past problems with anesthesia
If anything feels rushed, say so. You can ask the surgeon to slow down, repeat, or draw a picture. That is not rude. That is smart.
Pain Control and Anesthesia Choices
You have options for pain control. The right choice depends on your health, age, and the type of surgery.
Pain and Anesthesia Options for Common Office Procedures
|
Type |
What You Feel |
Common Uses |
Key Risks |
|---|---|---|---|
|
Local numbing shot |
Awake. Pressure, but no sharp pain in the numbed spot. |
Simple tooth removal. Small biopsies. |
Short-term lip or tongue bite. Rare allergic reaction. |
|
Local shot with oral pill |
Awake but calm. Some drowsiness. |
Multiple extractions. Minor implant work. |
Slower reaction time. You need a ride home. |
|
IV sedation |
Very drowsy. You may not remember the surgery. |
Wisdom teeth removal. Several implants. |
Breathing changes. Extra heart and lung checks. |
|
General anesthesia |
Fully asleep. Breathing support from a machine. |
Major jaw surgery. Complex facial repair. |
Higher risk for heart, lung, and throat problems. |
Your surgeon and anesthesia team should explain why one choice fits you. They should also describe what happens if there is a problem.
Common Types of Oral Maxillofacial Surgery
Many people face the same three groups of procedures.
- Tooth and wisdom tooth removal. The surgeon opens the gum, removes bone if needed, and takes out the tooth. You may need stitches. Swelling and soreness are normal.
- Dental implants. The surgeon places a small metal post in the jawbone. Later, a dentist adds a crown. Healing can take months.
- Jaw and facial surgery. The surgeon moves parts of the jaw to improve bite, breathing, or balance of facial features. This often needs a hospital stay.
Each of these has its own risks. They all carry some risk of infection, bleeding, or nerve injury.
How to Prepare Your Body
Your choices before surgery change your healing. Three steps matter for most people.
- Follow fasting rules. If you get IV sedation or general anesthesia, you cannot eat or drink for a set time before surgery. If you ignore this, your surgery may be canceled for safety.
- Manage medicines. Ask if you should stop blood thinners or certain diabetes drugs. Never stop on your own.
- Quit smoking. Smoking harms blood flow and bone healing. Even a short break before and after surgery helps.
The Centers for Disease Control and Prevention offers free tools to help you quit.
How to Prepare Your Home and Family
Recovery is easier when your home is ready. You can plan for three simple needs.
- Safe ride and support. You need a trusted adult to drive you home. You also need help for the first day if you had sedation or general anesthesia.
- Soft foods. Stock yogurt, soup, scrambled eggs, and mashed potatoes. Avoid crunchy or very hot foods at first.
- Supplies. Have ice packs, gauze, pain medicine from the pharmacy, and extra pillows for head support.
Children may feel scared when they see swelling or bruising. You can explain that swelling means blood is rushing in to help the body repair itself.
What Happens on Surgery Day
Most surgery days follow the same pattern.
- You check in and sign consent forms.
- A staff member reviews your history and fasting status.
- An IV may be placed for fluids and medicine.
- The surgeon marks the site and reviews the plan with you one more time.
After surgery, staff watch you until you can drink, walk with help, and talk clearly. Then they review written home care instructions with you and your escort.
Recovery: What You Should Expect
Healing time depends on the type of surgery. Still, many patients share three phases.
- First 24 hours. Bleeding slows. Swelling starts. Pain is strongest during this time. Use cold packs as directed.
- Days 2 to 3. Swelling often peaks. Bruising may show. Pain should start to ease with medicine.
- Days 4 to 7. Swelling goes down. Stitches may dissolve or be removed. You can add more normal foods.
Call your surgeon right away if you notice:
- Fever higher than the level listed in your instructions
- Bleeding that soaks gauze for more than one to two hours
- Sudden new pain after several better days
- Yellow or green fluid from the wound
- Shortness of breath or chest pain
Questions You Should Ask Your Surgeon
Clear questions give you power. You can bring this short list on your visit.
- What are my choices if I do not have this surgery now
- What are the three main risks for me
- Who will give and watch my anesthesia
- How many times have you done this exact procedure this year?
- What pain can I expect on day one, day three, and day seven
- When can I return to work, school, or sports
Moving Forward With Confidence
Oral maxillofacial surgery can feel frightening. Yet clear facts reduce fear. When you know how to prepare, what will happen, and when to call for help, you protect yourself. You also protect your family. You deserve time, respect, and honest answers from your care team. You have the right to ask questions until you feel ready to say yes.